Cough and cold are the most frequent symptoms seen in children
It has become a trend to keep medicines at home for cough and cold
Many Parents are in habit of giving self medications to their children without any knowledge of dose and frequency of admininstration
Moreover,the dose of medicines keeps on changing in children unlike in adults
Parents are giving cough and cold medications for other purposes also like while air travelling to sedate the baby.
Cough and cold medications containing DIPHENHYDRAMINE ,when given in excessive doses,act as stimulants rather than sedatives.
The preparation containing DIPHENHYDRAMINE has killed many children.
There is evidence that these medications do not lessen the severity or duration of cough and cold.
Maximum deaths have occured in children below 2 years of age
In many homes,children easily access these medicines
THESE MEDICINES SHOULD NEVER BE PRESCRIBED IN CHILDREN BELOW 2 YEARS OF AGE
REFERENCES:Pediatrics: “Pediatric Fatalities Associated With Over-the-Counter Cough and Cold Medications,” “Pediatric Poisoning Fatalities: Beyond Cough and Cold Medications.
Author: Pediatrician and Pediatric Pulmonologist Dr.Dev Kumar Jha,Formerly at AIIMS,New Delhi
How to differentiate Dengue fever from MIS-C,Dr.Dev,M.D.,Pediatrician and Pediatric Pulmonologist ,Mohan Nagar,Ghaziabad,Delhi NCR
Severe Dengue fever and Multisystem inflammatory syndrome in children(MIS-C) both are the states of cytokine storm
Both these conditions present almost similarly,clinically
In the period of September-October 2021 both disease conditions are being seen frequently in India
Severe Dengue fever is caused by Dengue virus ,transmitted into human through Aedes mosquito bites
MIS-C is a post COVID 19 state
It is very important to differentiate between these two conditions for the treatment purposes as the treatment of these two are entirely different
In cases of severe Dengue fever the mainstay of treatment is aggressive fluid therapy with crystalloid ,colloid and when needed ionotrops and platelet transfusion if severe thrombocytopenia.
In contrast,aggressive fluid therapy may be life threatening in MIS-C,in which there may be left ventricular dysfunction.In this condition, the mainstay of treatment is intravenous steroid with or without IVIG.Other medications required are low molecular heparin and aspirin.
If there is fever with prominent vomiting,myalgia,erthmatous rashes,profound weakness and on investigations there is leucopenia,severe thrombocytopenia,hemoconcentration and raised serum Ferritin,it is indicative of severe Dengue fever. Positive NS1 antigen and or IgM antibody for Dengue virus confirms the diagnosis
If there is conjuntival injections,swelling of hands and feet,altered sensorium and diarrhoea along with fever, and on investigations leucocytosis,fibrogienemia,raised serum D-Dimer,raised serum IL6 ,it is leading towards the diagnosis of MIS-C. Positive RT-PCR or antibody againt COVID 19 confirms the diagnosis.
REFERENCES:1.Indian Pediatrics:volume 58;15 october 2021
2. Ahmed M, Advani S, Moreira , et al. Multisystem
inflammatory syndrome in children: A systematic review. E
Clin Med. 2020;26:100527.
3. Mishra S, Ramanathan R, Agarwalla SK. Clinical profile of
dengue fever in children: A study from southern Odisha,
India. Scientifica (Cairo). 2016;2016:6391594.
Large population of Delhi NCR children have ASTHMA.Dr.Dev,MD,Pediatrician and Pediatric Pulmonologist,Ghaziabad,Delhi NCR
Delhi is among most polluted cities in the world
Air pollution directly affects lung
Lungs of children are most vulnerable as the lungs are growing.
Children breath in more air than adults due to fast respiratory rate as compared to adults
Particulate matters in air particularly PM10 and PM2.5 can enter the airways and PM2.5 can go into alveoli
The level of PM10 and PM2.5 are 15 times higher in Delhi air as compared to set standard by World Health Organisation
The pollutants in air comprise obesogenic compounds responsible for making a child Obese
Obesity is associated with the development of Asthma in children
According to a cross sectional study done in 3 cities in India including the most polluted city Delhi and 2 less polluted cities in South India-Kottayam and Mysore, Published in LUNG INDIA September-October 2021,approximately 30% children in Delhi are suffering from Asthma.
Almost 50% children reported cough and 30% complained of shortness of breath.
Among 4361 children studying in private schools between the ages of 13-14 and 16-17,boys and girls, 3157 successfully completed the ISAAC Questionnaire and performed spirometry.
On the basis of spirometry ,which shows airway obstruction, a diagnostic component of Asthma,almost 30% children were diagnosed as having ASTHMA.
Most of the parents and children are not aware of this disease in children.
They are not easily accepting the diagnosis of ASTHMA in children, but it is a fact and we should do something proactively to control the level of pollution in cities to control the ASTHMA
The study has been published in LUNG INDIA September-October,2021
REFERENCES;. Singh V, Singh S, Biswal A. Exceedances and trends of particulate matter (PM2.5) in five Indian megacities Sci Total Environ. 2021;750:141461
Cited Here | PubMed | CrossRef
2. Central Pollution Control Board, Ministry of Environment, Forest and Climate Change. National Ambient Air Quality Status and Trends. 2019 Available from: https://cpcb.nic.in/upload/NAAQS_2019.pdfLast accessed on 2020 Oct 28
Cited Here
3. The Lancet Planetary Health. . Government indifference over air pollution crisis in Delhi
UPCOMING WAVE OF COVID-19 and Children,Dr.Dev,M.D.,Pediatric Pulmonologist,Ghaziabad,Delhi NCR
The coronavirus disease and or infection has affected all age group of individuals all over the world.
The herd immunity ,means immunity of entire population of an area to fight any disease develops naturally when almost 70% population of that area is infected .
The other way to develop immunity against the disease is,vaccination of the entire population.
It has been in discussion in India for last couple of weeks that,the upcoming wave of COVID-19 will affect only children and there will be large number of deaths among children.
It has been observed till now all over the world that children have been affected lees and mortality has been less as compared to adults.
But fear among parents and among doctors is genuine.
There are two reasons for that.
1. Since the adult population has been widely covered by vaccination,they will either have no disease or less severe disease.Children are left unvaccinated till now ,so the infection will cause various degrees of diseases in children.
2.Although the mortality percentage is less in children as compared to adults,a large population of diseased children will put burden on health care system and as the number of diseased children will be more,there will be less medical care and high mortality
REFERENCES:Interview given by Dr. Bhramar Mukharjee,Professor and chair of biostatistics,Michigan school of Public health,published in TOI,Delhi edition,Friday,25.06.2021
PANEL DISCUSSION ON ASTHMA IN CHILDREN WITH OR WITHOUT COVID 19,by Experts,moderated by Dr.Dev,M.D,Pediatric Pulmonologist and Respiratory intensivist ,Delhi ncr
https://m.facebook.com/story.php?story_fbid=1406721312822521&id=412160705929917?sfnsn=wiwspwa&extid=jHdMecjhkGPw6XDM&d=w&vh=eAsthma is the most common chronic respiratory disease in children worldwide.
It is being discussed by international experts.Please click below
https://m.facebook.com/story.php?story_fbid=1406721312822521&id=412160705929917?sfnsn=wiwspwa&extid=jHdMecjhkGPw6XDM&d=w&vh=e
https://m.facebook.com/story.php?story_fbid=1406721312822521&id=412160705929917?sfnsn=wiwspwa&extid=jHdMecjhkGPw6XDM&d=w&vh=e
This is being published here to update the knowledge of doctors treating asthmatic child.
It should be translated into the better care of asthmatic children all over the world.
NEWER TESTS TO DETECT INFECTION WITH Mycobacterium Tuberculosis,Dr.Dev,M.D.,Pediatrician and Pediatric Pulmonologist,Mohan Nagar,Ghaziabad,Delhi NCR
The oldest and time tested test to detect Tuberculosis infection in an individual is TST(Tuberculin skin test),also known as Mantoux test.It is being done with PPD RT -23.The standard strength for its use is 2TU(tuberculin unit).
But this strength is not available in the market and pathologists are compelled to use 5TU,the cut off value of induration for which is not standarized.
Moreover ,there may be false positive results, due to cross reactivity with Mycobacteria other than Mycobacterium tuberculosis (NTM)and BCG Vaccination particularly if the vaccination has been done after the infantile period.
The latest test which will be available in market very shortly is C-Tb skin test.
C-Tb skin test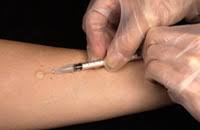
C-Tb test- This test is done in a similar manner as Mantoux test.Instead of PPD-RT23,in this test, antigens either ESAT6 or CFP 10 are used ,which are also used in Quaniferon Gold test.
This is the reason,it does not cross react with non tuberculous Myobacterium(NTM) as well as with BCG.At the same time, the test is not as complicated as Quantiferon Gold as it does not require sophisticated laboratory.
In the same way as in Mantoux test,0.1 ml of antigen is inoculated intradermally and the induration is meassured after 48-72 hours with ball pen and scale method. The cut off point has been established at 5mm for all age groups,irrespective of HIV status,irrespective of BCG Vaccine status.
The positive result indicates only the infection specifically to Mycobacterium tuberculosis but not the active disease
IGRA TEST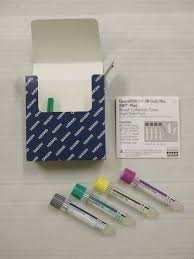
IGRA TEST:This test is interferon gamma release assay test.This is based on the principle that when T lymphocytes infected with Mycobacterium tuberculosis is exposed to specific antigen of M.Tb, in the form of either ESAT6 or CFP10 ,they release interferon gamma which is then measured.There are two tests,
QUANTIFERON TB GOLD ;In this test total interferon gamma which are released is measured
and
T spot TB. -It is a variant of Ellispot .In this test the number of effector T cells are measured which release interferon gamma upon exposure to specific antigens.
So ,this test is specific for Mycobacterium tuberculosis and it is not positive in cases of NTM(non tuberculosis mycobacteria) or in cases of BCG vaccination.
There is no need of a technique of intradermal inoculation and the measurement of induration as this test uses blood withrawn from patients.
There is no need of different cut off point of induration for HIV and non HIV patients
This test indicates only the infection,not the active disease
But ,this is not reliable below the age of 5 years.
REFERENCES:
1. World Health Organization. Guidelines on the management of latent tuberculosis infection. 2015. Report No.: WHO/HTM/TB/2015.01
2. Aggerbeck H, Giemza R, Joshi P, Tingskov PN, Hoff ST, Boyle J, et al. Randomised Clinical Trial Investigating the Specificity of a Novel Skin Test (C-Tb) for Diagnosis of M. tuberculosis Infection. PLoS ONE 2013;8(5):e64215 10.1371/journal.pone.0064215 [PMC free article] [PubMed] [CrossRef] [Google Scholar]
3.Hoff ST, Peter JG, Theron G, Pascoe M, Tingskov PN, Aggerbeck H, et al. Sensitivity of C-Tb: a novel RD-1-specific skin test for the diagnosis of tuberculosis infection. Eur Respir J 2015. December 17;47(3):919–28. 10.1183/13993003.01464-2015 [PubMed] [CrossRef] [Google Scholar]
4.Ruhwald M, Aggerbeck H, Gallardo RV, Hoff ST, Villate JI, Borregaard B, et al. Safety and efficacy of the C-Tb skin test to diagnose Mycobacterium tuberculosis infection, compared with an interferon gamma release assay and the tuberculin skin test: a phase 3, double-blind, randomised, controlled trial. Lancet Respir Med 2017. January 31;5(4):259–68. 10.1016/S2213-2600(16)30436-2 [PubMed] [CrossRef] [Google Scholar]
5. World Health Organization. Guidance for national tuberculosis programmes on the management of tuberculosis in children – 2nd ed. 2014. Report No.: WHO/HTM/TB/2014.03.
…
6.C-Tb skin test to diagnose Mycobacterium tuberculosis infection in children and HIV-infected adults: A phase 3 trial
PLoS ONE. 2018; 13(9)
7. Mori T, Sakatani M, Yamagishi F, Takashima T, Kawabe Y, Nagao K, et al. Specific detection of tuberculosis infection: an interferon-gamma-based assay using new antigens. Am J Respir Crit Care Med 2004. July 1;170(1):59–64. 10.1164/rccm.200402-179OC [PubMed] [CrossRef] [Google Scholar]
8.Sollai S, Galli L, de MM, Chiappini E. Systematic review and meta-analysis on the utility of Interferon-gamma release assays for the diagnosis of Mycobacterium tuberculosis infection in children: a 2013 update. BMC Infect Dis 2014;14 Suppl 1:S6. [PMC free article] [PubMed] [Google Scholar
9.Sensitivity of C-Tb: a novel RD-1-specific skin test for the diagnosis of tuberculosis infection.
[Eur Respir J. 2016]
10.Safety and efficacy of the C-Tb skin test to diagnose Mycobacterium tuberculosis infection, compared with an interferon γ release assay and the tuberculin skin test: a phase 3, double-blind, randomised, controlled trial.
[Lancet Respir Med. 2017]
11.Review Gamma interferon release assays for detection of Mycobacterium tuberculosis infection.
[Clin Microbiol Rev. 2014]
12.Specific detection of tuberculosis infection: an interferon-gamma-based assay using new antigens.
TERMS USED TO DESCRIBE RESISTANT TUBERCULOSIS,Dr.Dev,M.D.,Pediatrician and Pediatric Pulmonologist,Mohan Nagar,Ghaziabad,Delhi NCR
The burden of resistant tuberculosis is on the rise which is a threat to WHO END Tuberculosis programme .
Children are also becoming victim but data are not sufficient yet
Primary resistance:When an individual is infected with resistant strain of Mycobacterium tuberculosis
Secondary resistance:When an individual is infected with drug sensitive strain of Mycobacterium tuberculosis but during the course of treatment the organism acquire resistance due to suboptimal treatment,incomplete treatment with high bacterial load.It is also known as acquired resistance.
MONORESISTANCE:When the organism is resistant to only one drug
POLYRESISTANCE;When the organism is resistant to 2 drugs but not to both Rifampicin and Isoniazid
MULTI DRUG RESISTANCE(MDR): When there is resistance to both Rifampicin and Isoniazid
PRE EXTENSIVELY RESISTANCE(PRE-XDR):When there is resistance to Rifampicin,Isoniazid with resistance to either Fluoroquinolones or Second line injectables(SLI) but not to both.
EXTENSIVELY DRUG RESISTANCE:When there is resistance to Rfampicin ,Isoniazid and both Fluoroquinolones and SLI
RR Tb: When there is resistance to Rifampicin with or without resistance to other anti tuberculosis drug
SLI(second line injectables): Amikacin,Kanamycin and Capreomycin
REFERENCES:Indian Journal of Pediatrics,volume 87/number 10/October 2020
Tips to maintain good appetite in children,Dr.Dev,M.D.,Pediatrician and Pediatric Pulmonologist,Mohan Nagar,Sahibabad,Ghaziabad,Delhi NCR

A good appetite is gift of nature to every individual born on the planet.
As soon as the child is born ,he or she is hungry to take feeds.
Any child may not remain without taking feeds for a long time.
If the child is not hungry ,it is not natural.
A child with less appetite or loss of appetite is definitely suffering from some problems,either physical or psychological.
TIPS TO MAINTAIN APPETITE:
Do not feed the child very frequently as this practice inhibits the appetite centre of brain ,because you are not allowing time for this centre to be stimulated by hunger .
So, child should be given foods after a minimum gap of 2-3 hours.
Child should be given foods of their choice not of the choice of family members.
Child should never be forced to feed at a certain point of time if he or she is not interested to take feed at that time.
The food items should be well grinded so that any child may not have difficulty in manipulating it inside the mouth.
The child should be involved in outdoor play as long as possible so that their activities could be maximised which maintains the appetite.
There are some foods especilally zinc containing foods which increases the appetite.
These are -nuts like peanuts,almonds
Seeds like sesame seeds,pumpkin seeds
Cheese contains good amount of zinc.Beans contain good amount of zinc.
Child should be given foods with Indian spices in good quantity which increases appetite.
Every child should be exposed to household foods between the age of 6-12 months because this is the time of developing taste buds.By doing so,they will accept household foods in future during entire childhood period ,otherwise they will be more interested in foods from markets.
Child after the age of 1 year shuold not drink more than 500 ml of milk per day ,otherwise they will not be able to take the necessary elements as their stomach will be full of milk.
If the child is not interested in drinking milk,there is no problem,give them milk products like yoghurt ,cheese ,paneer which will meet the requirement as well as increase the appetite.
Never give tea or coffee to any child
DO not give fruit juices to children,instead give whole fruit after proper cutting or mashing as per the age of the child.
Avoid giving more oily foods as it may lower the appetite.
Loss of appetite is the feature of many diseases.So consult your doctor if the problem of less appetite persists.
Do not overfeed the child as it will increase the weight above the normal range making your child overweight or obese which is as bad as loss of weight.
NOTE; EVERY CHILD SHOULD BE GIVEN ONLY AND ONLY THE MILK OF MOTHER TILL THE AGE OF 6 MONTHS.
USUAL SYMPTOMS,UNUSUAL DIAGNOSIS,A CASE REPORT,Dr.Dev,M.D.,Pediatrician and Pediatric Pulmonologist,Mohan Nagar,Sahibabad,Ghaziabad,Delhi NCR
 11 years old female child presented to our clinic with complaints of
11 years old female child presented to our clinic with complaints of
Fever for 24 days,
cough for 15 days
less appetite for 10 days
pain abdomen for 7 days
headache for 5 days
swelling of both lower limbs for 3-4 days
On examination;
Temperature 103 dF,pallor +,icterus+
Pulse rate 56/m regular(relative bradycardia)
Respiratory rate 26/minute ,regular
Generalised lymphadenopathy
bilateral pedal edema
Abdomen-not distended,no tenderness,hepatosplenomegaly+
Chest-bilateral equal breath sound,bilateral vesicular breath sound,bilateral crackles
CVS-NAD
CNS-NAD
Following diagnoses were suspected
Malaria
Typhoid
Viral hepatitis with secondary bacterial infection
Disseminated tuberculosis
Leptospirosis
Scrub typhus
Investigations were planned and done accordingly.
Hb 9 gm/dl
TLC 6800/cmm,P56,L34,E03,M07,B00,Platelet 90000/cmm
SGPT-102,SGOT146,ALP 200,S.BIL 3.8mg/dl
Serum Sodium 130mE/L,Serum potassium 4.4mE/dl
Serum widal-negative
Malaria antigen-negative
Chest X-Ray -bilateral reticulonodular opacities with bilateral pleural effusion
Mantoux test-negative
GA for CBNAAT -negative
The child was emperically treated as enteric fever with cefixime but there was no response.Then the child was treated emperically for malaria and again there was no response.
At this point of time,it was suspected that the child may be suffering from scrub typhus as the child travelled to Uttrakhand during last month.
IgM ELISA for scrub typhus was sent and it came to be positive and the child responded well to doxycycline.
DISCUSSION
:Rickettsia is intracellular ,gram negative proteobacteria with coccobacillar shapes.The disease caused by it is called Rickettsiosis.It is a zoonosis ,transmitted into human by mites(chiggers),ticks or fleas and rodents. Humen are the incidental host.No human to human transmission has been observed.
This disease is frequently seen in Uttrakhand,Rajsthan,assam.West Bengal ,Jammu and Kashmir,Maharashtra Tamil Nadu and Kerala region of India and many countries out of India.
pathogens causing disease in human have been broadly classified into three groups
1.Spotted fever group
2.Typhus group
3.Scrub typhus group
Scrub typhus is causing a health impact in Asia
Pathogenesis;The principle pathogenetic mechanism is vasculitis involving medium and small vessels.It causes increased vascular permeability by disrupting the endothelial tight junctions due to the bacterial load and tumour necrosis factor.Main cause of mortality is pulmonary edema and cerebral edema.
CLINICAL FEATURES OF SCRUB TYPHUS WHICH IS COMMON IN INDIA:
The usual incubation period is 10-12 days with a variability of 6-21 days.Symptoms varies from mild self limiting to severe causing death.
After the period of approximately 5-6 days of bite by mites,there occurs the formation of ESCHAR(shown in the figure) at the site of inoculation of the mite.It is a painless necrotic lesion over skin resembling a cigarette burnt skin surface.The usual sites are groin,axilla,back,neck and other exposed parts of the body.Eschar, if visibl,e makes a clear cut diagnosis of scrub typhus without any investigation.But it is not ususally seen in children.Its prevalence varies from 7-80%.
After about 5-7 days flu like symptoms occurs.In most of the cases fever has been observed with severe headache.
There may be myalgia,weakness,pain abdomen,vomiting,diarrhoea,cough.
O/E There may be relative bradycardia,generalised lymphadenopathy,generalised body rashes and pedal edema
On systemic examination:there may be hepatosplenomegaly
On investigation:
BLOOD-there may be anemia,thrombocytopenia,raised liver enzymes,raised serum bilirubin,hyponatremia,raised blood urea and serum creatinine
Chest X-Ray may show reticulonodular opacities,features of pulmonary edema,bilateral pleural effusion
ECG may shows features of myocarditis with nonspecific ST-T changes,features of heart block
LUMBAR PUNCTURES :CSF pictures are indicative of meningoencephalitis.The CSF picture is similar to Tuberculous meningitis with lymphocytic pleocytosis and raised protein.
DIAGNOSIS; The gold standard is INDIRECT IMMUNOFLUORECENT ANTIBODY TEST(IFA), but it is not available everywhere.The next best is IgM ELISA which is widely available and should be done as the sensitivity of Weil-Felix test is very poor.
TREATMENT.The drug of choice is doxycycline,oral or i.v. in the dose of 2.2 mg/kg 12 hourly below 40 kg of weight and 100 mg b.d. above 40 kg of weight,for a period of 7 days of 3 days after the fever subsides.Now it has been recommended for children of any age to treat Rickettsial diseases as it has not caused enamel hypoplasia or teeth staining even after multiple courses.
Alternative medicine is Azithromycin in the dose of 10 mg/kg/day
Other drugs which may be used in special cases are -clarithromycin.chloramphanicol and Rifampicin
Mortality is above 50% if not recognised and treated timely
COMPLICATIONS.HLH(hemophagocytic lymphohistiocytosis and it is very serious complication.
REFERENCES:
AbdadMY,Abou AbdallahR,FoumierP-E,StenosJ,Vasoo S.Aconcise review of the epidemiology and diagnostics of rickettsioses:Rickettsia and Orientia spp.J clin Microbiol.2018;56:eo1728-17
IssacR,VargheseGM,MathaiE,et al.Scrub typhus:prevalence and diagnostic issue in rural southern India.Clin infect dis.;2004:39;1395-6
Rathi N ,Kulkarni A ,Yewale V;Indian Academy of Pediatrics Guidelines on Rickettsial diseases in children committee.IAP Guideline on Rickettsial disesase in children.Indian Pediatr.2017;54:223-9
Elisabeth BN,Cristina S,DidIer R,Phillipe P.Treatment of Ricketssial spp.infections:a review.Exp rev anti infect Ther.2012;10:1425-37
NASAL POLYP,WORKING KNOWLEDGE,Dr.DEV,M.D,Pediatrician and Pediatric Pulmonologist,Mohan Nagar,Sahibabad,Ghaziabad,Delhi NCR
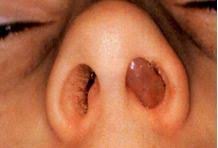 Nasal polyp is not uncommon in children and parents often get afraid of it when it is visible.
Nasal polyp is not uncommon in children and parents often get afraid of it when it is visible.
It is rare below the age of 10 yeras.
It is an abnormal growth which is semitransparent and may arise from any portion of nasal mucosa or epithelium of paranasal sinuses usually at its outflow.
Contrary to the common belief,it is associated more commonly with non allergic than allergic conditions.
It is seen more commonly in children with non allergic asthma than allergic asthma
It may be single or multiple depending on etiology.
CLINICAL FEATURES:
Small polyps are asymptomatic which are usually discovered during nasal examination for other causes,when they are located anterior to the anterior edge of middle turbinate
Symptoms depend on size and location of the polyp.
Small polyp arising from middle meatus may produce symptoms by blocking the outflow tract,causing chronic and recurrent sinusitis.
common symptoms are
Rhinorrhoea,
post nasal drip
facial pain
headache
toothache
hyposmia,
anosmia,
loss of taste,
blocked nose,
snoring.
When the size becomes large,it may cause obstructive sleep apnea
DIAGNOSIS;
Clinical examination is sufficient for the idendification of this lesion.Anterior rhinoscopy wll defines it.
Non contrast CT scan of nasal and paranasal sinuses are required to see the extent of lesions as in rare circumstances there may be malignant lesions.SO the imaging investigation of choice is non contrst CT scan.
CAUSES:
It arises due to chronic inflammation of nasal or paranasal mucosa,so it is commonly seen in children with allargic or non allergic rhinitis or sinusitis.
Multiple polyps are seen in children with cystic fibrosis,primary ciliary dyskinesia ,asthma and allergic fungal sinusitis.
TRATMENT:
Treatment is medical in most of the cases.Surgery is required only rarely when medical treatment fails.
In most of the cases ,short term oral corticosteroid and or intranasal steroid is needed.
REFERENCES:
Bernstein JM, Gorfien J, Noble B. Role of allergy in nasal polyposis: a review. Otolaryngol Head Neck Surg. 1995 Dec. 113 (6):724-32. [Medline].
Tos M, Sasaki Y, Ohnishi M, Larsen P, Drake-Lee AB. Fireside conference 2. Pathogenesis of nasal polyps. Rhinol Suppl. 1992. 14:181-5. [Medline
Rudmik L, Schlosser RJ, Smith TL, Soler ZM. Impact of topical nasal steroid therapy on symptoms of nasal polyposis: a meta-analysis. Laryngoscope. 2012 Jul. 122 (7):1431-7. [Medline].
Lund VJ, Flood J, Sykes AP, Richards DH. Effect of fluticasone in severe polyposis. Arch Otolaryngol Head Neck Surg. 1998 May. 124 (5):513-8. [Medline
Rudmik L, Schlosser RJ, Smith TL, Soler ZM. Impact of topical nasal steroid therapy on symptoms of nasal polyposis: a meta-analysis. Laryngoscope. 2012 Jul. 122 (7):1431-7. [Medline].